
Author Archives: Julie Philippart


Hip Adductor Length Test
I

Hamstring Length
I
Hamstring length: Gluteus maximus muscle weakness (as often described in Lower crossed syndrome) can lead the hamstrings muscles to act as primary hip extensors as compensation, leading to imbalance and faulty movement. There are several ways to assess hamstring length, but here just one of them is described as in Magee (2006).
The patient is supine with hips and knees in 90°. The examiner passively straightens the lower leg. Normal length of the hamstring muscle is 90° hip position with straight knee. Less than 80° is referred as loss of hamstring extensibility that can lead to gluteus maximus and quadriceps inhibition (Page et al, 1967).

Hip Abduction Test
I
Hip abduction: Meant to assess quality of the pelvic muscles and give information about the stabilization of the pelvis during gait. The test is performed with the patient lying on one side, the lowermost leg bent and one hand is flat on the table for stability. The patient is asked to abduct the uppermost leg (that is straight in relation to the trunk) about 20° and the examiner stands behind the patient to observe possible faulty movements.
The normal movement consist of abducting the leg straight up with no additional movements of hip, trunk and leg. A tight tensor fascia latae muscle will result in hip flexion, while an early lateral pelvic tilt is sign of atrophic gluteals because the muscle quadratus lumborum is acting before them (Page et al, 1967).

Leg Length Test
I
Leg length test: The patient lies supine. The examiner stands at the end of the table and palpates the medial malleoli at the same level on both sides. The patient is asked to flex knees and hips, and lifts the pelvis off the table and returns to the starting position. The examiner passively extends the legs and compares the height of both malleoli. Differing levels indicates asymmetry of the legs.

Leg Lowering Test
I
Leg Slide and Leg Lowering tests: Performed to assess the lower abdominal muscles that are not carefully assessed with the trunk curl up. The test can be done in two different ways according to your strength capacity. Normally the easiest is performed first.
The subject is in supine with knees bent and posterior pelvic tilt. Then, the patient is asked to straighten one leg at the time, keeping the heel in contact with the table and attempting not to lose the posterior tilt. If too easy, the patient can try both legs simultaneously.
If also the latter is deemed possible, then the patient is asked to perform the leg lowering test. The patient is supine with lumbar spine flat on the table (posterior pelvic tilt), knees extended and leg in 90° position. At this point, the legs are slowly lowered to the table without curving the spine. As soon as anterior tilt is detected the test is stopped and evaluated as positive (Kendall et al, 1993; Norris, 1995).

Painful Catch Sign
I
Painful catch sign: The patient lies supine and the therapist lifts both lower extremities by the ankle. The knees are kept extended and the therapist releases the ankles. The patients attempts to hold the legs up, and if the lower extremities fall instantly over the table because of back pain, the test is positive for lumbar instability. Watch also for jerky, painful movements while the patient lowers their legs to the table.
Note: The original test requires the patients to lift the legs on their own, but many patients with a lumbar instability will find it too difficult.
Reported to have 37% sensitivity and 73% specificity (Kasai et al. 2006).
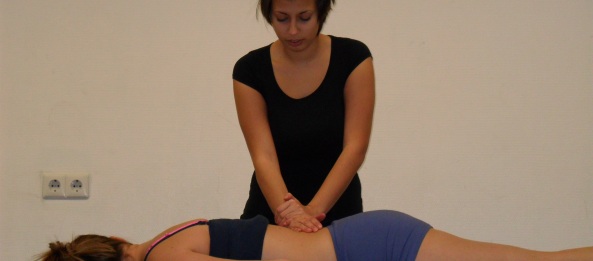
Passive Accessory Intervertebral Movements
I
Passive accessory intervertebral movements (PAIVM): Patient lies prone and the therapist tests intervertebral motion. The therapist places the hypothenar on the spinous process and moves the spinous process in an anterior-posterior motion. Each segment’s mobility is judged as normal, hypermobile or hypomobile, noting the presence of pain during the movement. Alqarni et al. (2011) suggest a standardization of the test to increase reliability.
Reported to have low sensitivity; 29% (Abbott et al. 2005), to 46% (Fritz et al. 2005), but a high specificity of 81% (Fritz et al. 2005) to 89% (Abbott et al. 2005).

Passive Lumbar Extension Test
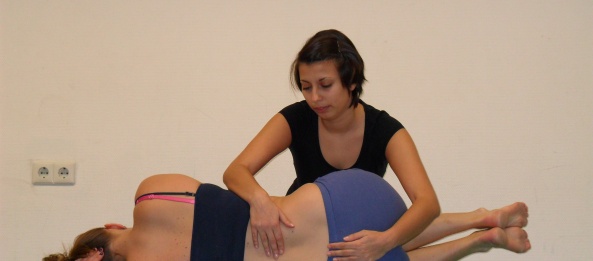
Passive Physiological Intervertebral Movements
I
Passive physiological intervertebral movements (PPIVM): Patient is in sidelying position. Hips and knees are flexed while the knees are locked, and the therapist moves the patient’s spine through flexion and extension movements. Therapist palpates between the spinous processes to assess the motion as normal, hypomobile or hypermobile.
This test should not be used to assess the entire lumbar spine’s mobility, and should not be used as a single examination technique (Shreiner, 2008). Reported to have a 5% (flexion) and 16% (extension) sensitivity and 98% (extension) 99.5% (flexion) specificity (Abbott et al. 2005).